
What the heck is a Carve-in?
It is the opposite of what Hospice providers have enjoyed for the past many years - the Carve-out! Currently, Medicare beneficiaries who have Medicare Advantage (MA) Plans revert to traditional Medicare when they elect the Medicare Hospice benefit - thus, they are “carved out” of MA plans.
The Medicare Advantage Carve-in Demonstration Project begins in 2021 and Hospice will be “Carved-in” and become part of Medicare Advantage plans. This is part of CMS’ recently announced expansion of the MA Value-Based Insurance Design (VBID) model. In addition to bringing hospice into the MA Plans the demonstration project will also cover expanded telehealth, services that address social determinants of health (meals, transportation and other QOL elements), advanced care planning, and hopefully, improved access to Palliative Care. (Jim Parker, Mar 2019, Hospice News)
So - what’s the point for me, a hospice team member?
There will be challenges to overcome and processes to put into place to deal with this new reimbursement system and increased oversight by insurance providers.
In 2019, CMS expects 22.6 million or 37.6% of Medicare beneficiaries will be enrolled in a Medicare Advantage plan. Examples of MA Plan providers include: Humana, United, Cigna, Aetna, Kaiser, BCBS, etc.
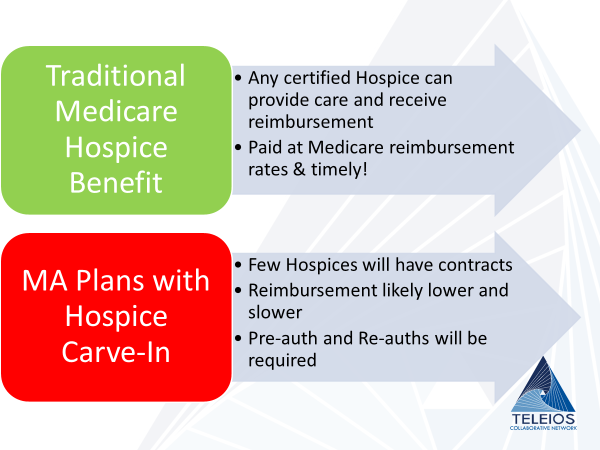
What does this mean for me at the bedside in 2021 when the Carve-In happens?
- Keep track of insurance coverage requirements – all Medicare patients will not be treated like traditional Medicare hospice beneficiaries.
- Be in frequent communication with the MA Plan’s hospice case manager.
- Have a system and people in place to get needed authorizations timely.
- Be sure documentation supports the need.
- Understand that the MA Plan is a very important customer.
To answer the question posed at the beginning – The Medicare Advantage Carve-in is a new hospice Reimbursement model that will require some major rethinking of our processes, our communication, and our expectations.
Being at the negotiation table with MA Plan administrators NOW to ensure we have a place in their network in 2021 is essential. This is one the very reasons that Teleios Collaborative Network exists – to bring negotiating power and influence to these conversations and inclusion in MA Plan contracts.
In addition, we must all expect a reduction in our reimbursement rates as the MA Plans make arrangements with hospice providers. These contracts will require high quality outcomes and care to be provided at lower cost. Depending on penetration of Medicare Advantage plans in our local areas, some hospices with higher populations of MA enrollees could see significant reimbursement cuts (10-25%)!

Janelle McCallum, RN, BSN, MSM
Chief Clinical Operations Officer & Coach
Teleios Collaborative Network


Teleios University (TU)
Program Launch: January 20-21, 2020

An organizational model that allows not-for-profit hospices (Members) to leverage best practices, achieve economies of scale and collaborate in ways that better prepare each agency to participate in emerging alternative payment models and advance their charitable missions.








